Search
Categories
- All
- Anesthesiology
- Breast Surgery
- Cancer Center
- Dermatology
- Ears, Nose, and Throat
- Emergency Room
- Endocrinology
- Family Medicine
- Fertility Clinic
- Gastroenterology
- General Surgery
- Gynecology
- Internal Medicine
- Laboratory
- Medical Imaging
- Nuclear Medicine
- Nutrition
- Obstetrics
- Ophthalmology
- Stomatology
- Orthopedics and Sports Medicine/Rehabilitation
- Pediatrics
- Pharmacy
- Psychology
- Respiratory Medicine
- Surgery
- Vasculocardiology
- PCR test (incl. bilingual report service fee)

How to use Fentanyl Transdermal Patches
LEARN MORE*What is this drug used for?
It is used to ease moderate to severe chronic pain. This drug is only for use by people who have been taking pain drugs (opioids) and are used to their effects.
*How to use Fentanyl Transdermal Patches?
1. Wash and dry the area of skin where the patch is to be applied. Do not use talc, oil, moisturisers or creams as this may prevent the patch sticking.
2. Tear open the patch package where indicated (use the fingers rather than scissors to prevent accidental damage to the patch). Damaged patch may cause overdose and death.
3. Remove the protective backing from the patch. Try not to touch the adhesive with fingers.
4. Press the adhesive side of the patch to the prepared skin site firmly. Ensure that there is good skin contact, particularly at the edges of the patch.
5. Wash hands thoroughly with soap and water to remove any possible contamination with medicament.
6. Replace this patch every 72 hours.
*What are some side effects that I need to call my doctor about right away?
1. Signs of an allergic reaction: like rash; itching; redness, swollen etc.
2. Severe constipation or stomach pain. These may be signs of a severe bowel problem.
3. Trouble breathing, slow breathing, or shallow breathing.
4. Trouble controlling body movements.
*Warning and caution!
1. The patch may have metal. Take off the patch before an MRI.
2. Take this drug off of the skin as you have been told before having certain tests like CT scans, MRIs, and X-rays.
3. If you have a defibrillator or pacemaker, talk with your doctor.
*What do I do if I miss a dose?
1. Put on a missed patch as soon as you think about it after taking off the old one. Do not apply double dose or extra doses.
2. If it is close to the time for your next dose, skip the missed dose and go back to your normal time. Do not use 2 doses at the same time or extra doses. Many times this drug is taken on an as needed basis. Do not take more often than told by the doctor.
*Storage conditions
1. Store at room temperature. Do not freeze.
2. After you take off a skin patch, be sure to fold the sticky sides of the patch to each other.
3. Safe-keep the used patch at your home. By law you must return the used patch to the hospital pharmacy for proper and safe disposal.
Reference:
1. Fentanyl Transdermal Patches Package Insert
2. Applied Pharmaceutical Practice(2009)
3. Up to date
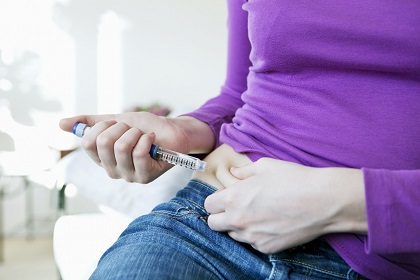
How to Self-Inject Low-Molecular-Weight Heparin
LEARN MOREStep 1: Wash and dry your hands thoroughly.
Step 2: Sit or lie in a comfortable position and choose an area on the right or left side of the abdomen, at least 5cm from the belly button. Avoid bruised, swollen, scarred, and sore areas.
Step 3: Clean the injection site with an alcohol swab and let dry.
Step 4: Remove the needle cap by pulling it straight off the syringe. Do not touch the needle once the cap is removed to keep the needle sterile.
Step 5: Hold syringe like a pencil in your writing hand
Step 6: Pinch an inch (2-3cm) of the cleansed area to make a fold with the other hand. Insert the full length of the needle straight down at a 90° into the fold of skin. The skin fold should be held throughout the injection.
Step 7: Press the plunger with your thumb until the syringe is empty and keep for 5 seconds.
Step8: Pull needle straight out at the same angle that it was inserted, and release skin fold. Do not rub or hot compress the injection site to minimize bruising.
Step 9: Point needle down and away from yourself and others, and push down on plunger to activate safety shield.
Step 10: place the used syringe in the sharps box. Bring it to hospital for proper disposal.
Reference: 2018 Lovenox Enoxaparin Instructions for Self Injection

How to use eardrops
LEARN MORE1. Wash your hands thoroughly with soap and water.
2. If the drops are a cloudy suspension, shake the bottle well.
3. Tilt the affected ear up or lie on your side. For adult and to a child older than 3 years of age, pull the ear backward and upward ,or if giving to a child younger than 3 years of age, pull backward and downward to open the ear canal.
4. Instill the correct number of drops in your ear. Gently press on the small skin flap over the ear to help the drops to run into the ear canal. Keep your ear tilted for 5 minutes or insert a soft cotton plug in your ear.
5. Keep this position for 5 min, then turn head to make the affected ear toward ground. Let the liquid flow out.
Remember
The mouth may feel bitter, do not be alarmed, because the middle ear is connected to the pharynx, a small part of the liquid medicine will enter the mouth.
Reference
1. http://www.safemedication.com
2. 中国药师协会《实用患者用药指导》(人民卫生出版社)

How to use vaginal suppository
LEARN MORE1. Clean your hands. Use a mild soap to gently wash the outer parts of your vagina and the area around it.
2. Remove any external foil or plastic packaging from the suppository or cream.
3. If an applicator is provided, load the applicator as directed by the instruction.
4. Stand with one leg on a chair or lie down with knees bent and legs apart.
5. Press the applicator to insert the suppository or cream into the vagina. If no applicator is provided, use your forefinger to push it as far as is comfortable and make sure the suppository is in your vagina.
6. Wash the applicator and get ready for next use. Wash your hands.

How to use suppository
LEARN MORE1. If possible, go to the toilet and empty the bowels before use.
2. Wash your hands.
3. Remove foil or plastic wrapping.
4. Warm the suppository in hands to aid insertion.
5. Lie on your side with your lower leg straightened out and your upper leg bent forward toward your stomach.
6. Gently insert the suppository into the rectum with your fingers (push the suppository as far as possible), lower your legs and hold buttocks together to ensure retention. Unless the suppository is a laxative, it is best not to defecate for an hour.
7. Wash hands again.

How to use Nasal Sprays
LEARN MORE1. Gently blow nose to clear nostrils.
2. Wash hands with soapy water before using the spray.
3. Remove the cap from the spray.
4. Gently shake the spray. If using it for the first time, shake and spray it into the air several times to ensure that it is in good condition.
5. Tilt head slightly forward (look down at feet).
6. Close one nostril; gently press against the side of the nose with one finger.
7. Insert tip of nasal spray into open nostril and slowly breathe in through the open nostril, and while breathing in squeeze the spray to deliver one dose. It is important to keep the spray upright (do not sniff hard as the spray will travel straight to the back of the throat, failing to deposit any medication in the nostril).
8. Remove spray from the nose and breathe out through the mouth. Tilt head backwards for about a minute to prevent the liquid spray running out of the nose. If two puffs of a nasal spray are to be applied to each nostril, try to aim in a slightly different direction with each spray to cover as much of the lining of the nose as is possible.
9. Repeat in other nostril as directed. Nasal sprays may cause an unpleasant taste when draining into the throat. A drink of water will help remove the taste.
10. Dry the nozzle with a paper towel ,replace cap on spray.
11. Try not to blow nose for several minutes after using the spray.
Reference:
《 药学实践 Applied Pharmaceutical Practice》
Photo:http://erke.woman91.com/xiaoertuomin/20160621168545.shtml
https://www.haodf.com/zhuanjiaguandian/dengyean_7689608093.htm
How to use Turbuhaler
LEARN MORE1. Unscrew the cap and take it off. Hold the inhaler upright
2. Twist the colored grip of your Turbuhaler in any direction as far as it will go, and then twist it all the way back. You should hear a "click"
*For first time use, please do Step 2 twice
3. Breathe out away from the device
4. Place the mouthpiece between your teeth, and close your lips around it. Breathe in forcefully and deeply through your mouth
5. Remove the Turbuhaler from your mouth. Hold your breath for 5 seconds before breathing out
6. If you need a 2nd dose, repeat steps 2 to 5. When finished, replace the cap
7. After using, rinse your mouth and gargle with water, then spit out. Don’t swallow
8. The number in the side counter window indicates the number of doses left. When a red mark appears at the window, this means that your medication is running out. Please replace one immediately
Oseltamivir (Tamiflu) Patient Education
LEARN MOREIn the absence of oseltamivir granules available, adults, adolescents or children who cannot swallow capsules can use this capsule to prepare oral suspension for use.
Please follow the method below to make sure the accuracy of dose:
1. Hold a 75mg capsule above a small measuring cup. Carefully open the capsule and pour the powder into the measuring cup.
2. Use a calibrated syringe to add 5ml water to the bowl and stir for about 2 minutes.
3. Use syringe to extract the correct amount of mixture (in ml) according to dosage instructed by your doctor from the measuring cup.
4. Do not ingest undissolved white powder as these are inactive ingredients. Push the plunger of the syringe and pour the mixture into the second measuring cup. Unused mixtures should be discarded.
5. In the second measuring cup, add a small amount (up to 5ml) of sweet food, and mix with the mixture (to cover the bitter taste).
6. Mix well and give all to patient. The mixture should be swallowed immediately after preparation. If there is any mixture left in the bowl, rinse with a small amount of water and give to patient to drink.
Repeat each time if you need to take the medicine.
*Administration instruction (oral):
(1) Oseltamivir can be taken with or without food;Take it with food to relieve stomach discomfort;
(2) For the treatment of influenza a and b, treatment should be started within 2 days (ideally within 36 hours) of the onset of flu symptoms.
*Storage conditions:
◆ Store in a dry place. Do not store in the bathroom.
◆ Keep all medications in a safe place and out of reach of children and pets.
*What do I do if I miss a dose?
• Take a missed dose as soon as you think about it.
• If it is less than 2 hours until your next dose, skip the missed dose and go back to your normal time.
• Do not take 2 doses at the same time or extra doses.
Reference:
1. Oseltamivir(Tamiflu)Package Insert
2. Up to date
3. Influenza diagnosis and treatment guide (China 2011)
4. Applied Pharmaceutical Practice(2009)

How to use a Valved Holding Chamber
LEARN MORE1. Check that the holding chamber is in good condition, without any foreign objects. A damaged holding chamber cannot be used
2. Remove the INHALER DEVICE cap
3. Shake INHALER DEVICE canister vigorously for about 5 seconds. If using INHALER DEVICE for the first time, shake and spray the INHALER DEVICE into the air 1 to 2 times to ensure that it is in good condition
4. Insert the INHALER DEVICE into the back-piece of the holding chamber
5. Ask your child to sit in an upright position, and tilt their head back slightly towards the ceiling
6. Hold the INHALER DEVICE and holding chamber correctly as shown below
7. Apply the mask to your child’s face, ensuring an effective seal around the mouth and nose. Ensure there are no foreign objects in the mouth
8. Press the INHALER DEVICE with your thumb to release the medicine
9. Ask your child to breathe normally for 10 to 15 seconds, Please do not remove the mask until you have finished 10 to 15 seconds of breathing
10. Administer 1 puff at a time. Wait for about 15 to 30 seconds before the next puff.
11. Repeat steps 3 to 10 for the next puff
12. Remove the mask from the child's face
13. Ask your child to rinse his/her mouth, wash their face with water after use and Make sure the child will spit out the mouthwash
14. Re-cover INHALER DEVICE
How to clean and store a Valved Holding Chamber:
Clean the holding chamber before using it for the first time. Then clean the holding chamber weekly or biweekly
1. Remove the parts of the holding chamber (Don't take off your mouthpiece! B1, figure 1)
2. Soak the parts for 15 minutes in a mild solution of liquid dish detergent and lukewarm (around 40°C) clean water
3. Agitate it gently and clean all parts
4. Rinse parts in clean water, if necessary, use tap water to gently flush the one-way valve (B2, figure 1) back to the original position
5. Shake out any excess water from the parts, and allow them to air-dry in a vertical position
6. Ensure that the parts are dry before reassembly
7. Storage temperature: 5°C to 55°C, relative humidity of no more than 90%, cool and clean indoor environment
Reference: 1 Chamber insert
2 Uptodate patient education

How to prepare Potassium Permanganate External Solution from the tablet
LEARN MOREPotassium permanganate external solution is used to cleanse wounds and dermatitis skin conditions.
Preparation must be freshly made before use. The solution will appear pink or purple in color.
Be careful when handling this tablet and solution as it can permanently stain clothing and surface touched.
Different concentrations may be used as prescribed by your doctor.
Pharmacist to tick √ on the correct concentration for patient according to prescribed strength:
○ Concentration 1:10,000 (0.01%)
- Dissolve 1 tablet in 1000ml (1 liter) of warm water
- Sitz bath for topical treatment
Instruction:
- Fill the basin just short of full
- Soak the affected area for 5 to 10 minutes or as directed by your doctor.
- Dry the area with a clean towel that you don’t mind changing color.
- If the solution gets on other areas of your skin, wash with soap and water.
○ Concentration 1:4,000 (0.025%)
- Dissolve 1 tablet in 400ml of warm water
- For acute dermatitis, eczema and other skin condition
Instruction:
- Soak the gauze or sterile cotton ball into the prepared solution to apply on the affected skin area as wet dressing.
- The affected area can also be directly soaked into the prepared solution
○ Concentration 1:1,000 (0.1%)
- Dissolve 1 tablet in 100ml of warm water
- For wound cleansing
Instruction:
- Soak the sterile cotton ball or cotton tip in the prepared solution to clean the affected wound.
Warnings
1. External use only, do not take orally.
2. Irritant to mucosal membranes
Ref: Product package insert, British National Formulary
- First page
- Previous page
- ...
- 3
- 4
- 5
- 6
- 7
- ...
- Next page
- Last page









